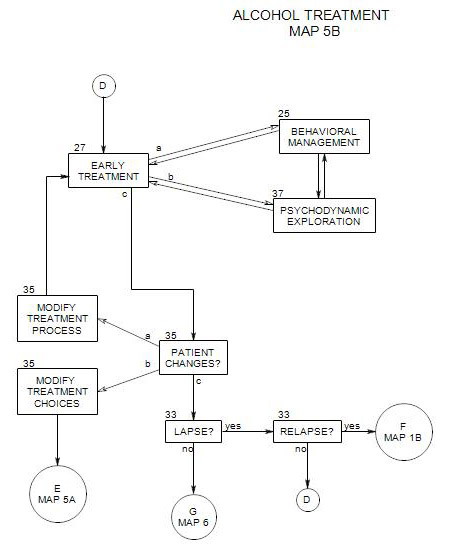
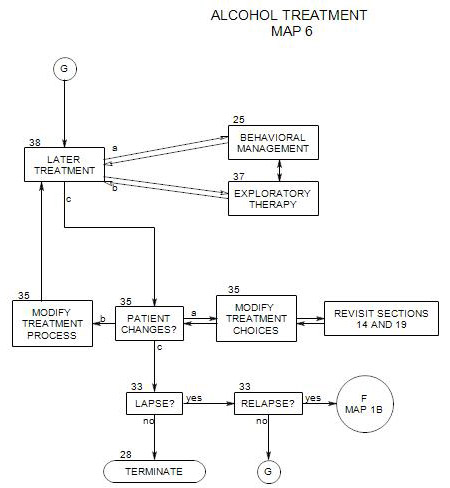
19. ADJUNCTIVE CARE DECISION
- This section should be used together with either Section 14 on Map 5, which has to do with choosing the primary mode of outpatient treatment, or with Section 27, which has to do with early treatment.
Commonly, the choices of primary and adjunctive forms of treatment are made with the patient as part of a comprehensive [formal or informal] treatment plan at the beginning of treatment. Alternatively, choice of adjunctive care can be deferred until the primary treatment is in progress and the patient’s additional needs become clear. In either case, adjunctive care choices can be revised as the patient changes or new information about him/her comes to light.
This section considers a variety of resources for diagnosis and treatment of alcohol misuse, any or all of which could be helpful with a specific patient. These include
- involving others
- family and friends
- professional consultations
- adjunctive psychotherapy
- living and working conditions
- self-help groups
- additional treatment and support
- the process of choosing adjunctive care
Adjunctive treatment can be crucial to the person’s ability to manage without drinking. Therapy can be a place where the effectiveness of other treatments and life-style changes are examined, evaluated, and coordinated.
19a. Making Referrals and Involving Others
Often a therapist will feel a tension between two approaches – the “take-charge”, or “medical” model in which the professional tells the patient what to do and where to go, and a “hands-off”, psychodynamic approach in which the professional makes suggestions or discusses issues with the patient and leaves the patient with the responsibility of following up. The choice of which route to follow in handling adjunctive care depends on the patient’s needs and abilities. If we are too prescriptive with patients who need their autonomy or are in an early stage of change, they are likely to react negatively to our choices for them. From the psychodynamic perspective, we are infantilizing patients. From the perspective of motivational interviewing, we are likely to drive patients away.
On the other hand, at this point in treatment, many alcoholic patients are unable to follow up adequately on referrals or the involvement of friends and family, or believe that they are unable to do so.
Making the referral should be negotiated with the patient and the patient’s reasons noted. This choice is part of your real relationship with the patient and can be a mine of information about his/her strengths, limitations and fears.
Patients may want you to make contacts because they
- feel weak and disoriented, and welcome your help.
- are uncertain and lack information. In this case, the issue becomes whether more information [names, telephone numbers, addresses, suggestions about approaches, etc.] will help, or whether the patient will still be unable to follow through.
- have fears or low self-esteem and doubt their ability to follow through.
- don’t see the point to the referral or don’t care enough to take action.
A patient may insist on making his/her own contacts because he/she
- is unable to accept any help and has to do it him/herself.
- doesn’t trust you yet- your motives, ability, or level of caring.
- thinks he/she can do things better than others, including you.
- can in fact be more successful than you, especially with family and friends.
A particular patient may feel comfortable making some of the contacts and not others, or may legitimately be better suited to making some contacts and not others.
Whenever the patient makes the contact for adjunctive care, it is helpful to follow up with him/her, to see how the contact went, decide what to do next, provide supplementary contacts or alternative adjunctive care. The results can also be input to the psychodynamic process [as for example, when the patient’s attempt to make contact leads to childhood associations or overuse of ego defenses] or behavioral work [as when it becomes clear that assertiveness training could be helpful in making future contacts].
When the therapist makes the contact, the patient will need to know the next step: how to follow through, what you will be doing next, and so on.
Contacts can also be made from the therapist’s office during a treatment session or consultation. The therapist can make the call while the patient observes and provides information about him/herself; or the patient can make the call with the therapist providing information and support as needed.
19b. Family and Friends as Adjunctive Support
The other people in a patient’s life can be his/her richest resources, or they can undermine the treatment. They are already present, they are involved, and they care about the person.
At any time during treatment, the support and cooperation of others in the patient’s family can be of value, by
- providing information about the patient’s behavior.
- setting a context that discourages drinking, for example, by keeping alcohol out of the house, not drinking themselves, discouraging the patient from having a drink, etc.
- joining with others in the family to put pressure on the patient not to drink.
- refusing to enable the patient’s drinking behavior in other ways.
- confronting the patient about drinking, so the drinking continues to be an active issue that he/she must deal with.
- acknowledging and supporting the patient’s efforts to deal with drinking and other issues.
Family members can be approached and asked for help, either by your patient or by you on your patient’s behalf. It may also be that they need help in a variety of ways, through education about the patient’s difficulties or through their own individual or family therapy.
You can’t assume that family and friends will be allies in treating your patient, however, for several reasons:
- They may not see a problem.
- They may have their own psychological problems that require their attention.
- They may be preoccupied with their own drug or alcohol issues.
- They may want the patient to change in other ways but to continue drinking with them.
- They may be angry at your patient for past behaviors or bitter about unfulfilled needs and fantasies.
- They may have adapted to the patient’s drinking and consequences, such as being absent or irresponsible. They may be reluctant to allow the patient to participate more or assume responsibilities.
- They may be blaming and judgmental and your patient is the identified problem source in the family.
- They may fear a change of involvement with a patient who has been violent, destructive or otherwise dangerous in the past.
- The family as a whole may be conflictual, competitive, impoverished or otherwise broken.
Family and friends can also undermine the patient’s treatment, by
- refusing to see change, even when it is occurring.
- blaming the patient for all that is wrong in the family or relationship.
- not recognizing their own issues and their own contributions to the patient’s pathology.
- enabling the patient’s self-destructive behavior in the guise of helping.
The patient may be from an alcoholic family, an alcoholic friendship group, or an alcoholic culture that not only contributes opportunities, behavior models and social approval for drinking but also resists any attempt by the patient to abstain. Treatment may involve helping the patient escape from social pressures to drink, in addition to dealing with his/her own internal pressures.
Family and friends can be enlisted to help in many ways:
- You can see them separately in the context of the patient’s treatment, as an explicit resource that you encourage and sustain.
- You can invite them into the patients’ sessions from time to time, to “check in” and see how things are going at home.
- They can provide emotional support.
- They can help the patient manage legal limitations, such as loss of a driver’s license.
- Early on, family members can, with the patient’s s cooperation, provide external controls on the patient’s impulse to drink, by controlling the patient’s money or ability to travel, or by keeping track of the patient at critical times when s/he is most likely to drink or get alcohol to drink later.
On occasion, you may want to encourage people close to an alcoholic to get in touch with one another, so they don’t each feel isolated and alone with the problem. They may find that they have similar reactions, and can support each other, even without further professional help. They may join together to put pressure on the alcoholic to change [ Section 22 ], and/or to arrange an intervention [ Section 13 ].
In addition, others who are most closely involved with the patient may be encouraged to seek their own treatment, for a variety of reasons
- They are under some of the same pressures as the patient, and could use help dealing with their own issues.
- They could use professional help in dealing with the patient.
- They may be contributing to the patient’s problems and should be focused on their own issues as a way to relieve some of the patient’s pressures. In fact, the identified patient may in some cases be simply the weakest link, with others who need help hiding behind the patient’s symptoms.
For example, If a couple are in serious financial difficulties, the wife may become critical of the husband for his failings. He then gets into the habit of stopping by a bar on the way home, to brace himself for her criticisms. She reacts to his drinking when he should be working or helping out at home, and they devolve into a vicious spiral in which he is the identified failure and she has no effective recourse.
If other family members are unable or unwilling to go for their own therapy, they may be encouraged to join self help groups, such as Al-Anon or Al-a-Teen, where they can learn from and share with others who are dealing with similar issues in their families.
If others are brought into a therapy setting that has previously been individual treatment, the patient should be warned that the therapist’s role will change in that setting. Some prediction of the change can be helpful to a patient – to expect you to be a little more distant and less supportive, for you to spend a lot of the time with the other person, etc.
In any case, the decisions about whether and how to make use of family members should be made with your patient. See Section 21 for more on this issue.
19c. Professional Consultations
A wide range of professionals may potentially be available to help in the treatment process. However, they may be expensive and may or may not be covered by a patient’s medical insurance. They include:
- nutritional counseling
- medical consultations
- psychiatric consultations
- drug testing
- couple therapy
- family therapy
- group therapy
NUTRITIONAL COUNSELING
Ongoing misuse of alcohol results in loss of appetite and gastroenterological distress and disease. In the short run, there can be consequences for a person’s energy level, mood, sleep patterns, and ability to focus and concentrate. In the long run, these can lead to malnutrition that in the extreme can be life threatening. Some of the results are reversible, others are not; and the consequences can result in damage to the body that endures into recovery. Nutritional counseling can help reverse some of these consequences by helping the patient develop and maintain a healthier diet.
MEDICAL OR PSYCHIATRIC CONSULTATIONS:
A physician referral may be of value in dealing with the alcohol misuse directly or in handling some of its consequences. Often a patient’s physician doesn’t know that the patient is drinking, and it can be of value to make the contact (with the patient’s knowledge and permission). Initial contact with the patient’s physician was discussed in Section 30 . At this point, more information may be available, including medical work carried out in detox or rehab, and another contact with the patient’s physician might be in order.
Sleep difficulties may need to be addressed medically. Commonly, people have trouble sleeping during early recovery, and may be tempted to have a drink to get needed rest. There are medications that induce drowsiness, especially hypnotics (e.g.: Ambien™), or antihistamines (e.g.: Benedryl™).
There may be medical consequences of drinking that need to be addressed, depending on how heavy and long-term the patient’s drinking may have been. Discussion of these issues can be helpful to the patient, and may uncover useful information that the patient might otherwise not mention to his/her physician.
Early stage chronic use of alcohol can result in headaches, gastritis, or interrupted sleep because of frequent nocturnal urination.
Middle stage alcohol use can result in loss of appetite, peptic or duodenal ulcers, esophageal reflux (periodic back-up of food causing burning sensation in throat), etc.
Late stage alcohol use may result in neuropathy (loss of sensation in fingers and toes), esophageal varices (varicose blood vessels in the throat from constant irritation of alcohol), significant weight loss, etc.
When psychological issues are involved, a psychiatrist may be better able to diagnose and prescribe medications for your patient. These include
- use of medication to manage a patient’s anxiety or depression.
- combinations of alcohol misuse and another psychiatric diagnosis that requires medication.
- a person who drinks in part because the right psychotropic medication or combination of medications has not yet been tried.
- a patient who is already using other psychotropic medications that must be dealt with in the light of his/her alcohol misuse.
Any physician who prescribes medications should be aware of the patient’s alcohol issues. Another discussion of the use of psychotropic medications to deal with psychological issues appears in Washton and Zweben, 106-108
For some patients, medication may be helpful in reducing drinking or achieving or maintaining abstinence. The options can be discussed with the patient, followed by a consultation with a physician or psychiatrist. Some of these medications are discussed in Section 48.
DRUG TESTING
If a patient is using other drugs in addition to alcohol, then voluntary drug testing may be of some value in helping him/her stay straight. However, it is less valuable in this way for alcohol, because the tests are generally not reliable and alcohol leaves a person’s system so quickly that he/she can continue to drink and test negative.
If testing has been legally mandated – most likely following a driving incident – then going for the tests is an emotionally loaded event, and worthy of exploration in psychotherapy. The testing situation itself may be perceived as demeaning, and a patient may need help in coping. It is too easy to avoid going, forget, arrive angry, or engage in self-defeating behaviors relative to the testing situation or the officer in charge.
Tests are typically random, and the patient must check every night to learn whether he/she is required to go for testing the next day. He/she must remain within travel distance of the testing facility and get special permission from a judge to leave for vacation or any other reason. This is a constant reminder of his/her actions while drinking, which can be processed in psychotherapy.
19d. Adjunctive Psychotherapy
COUPLE OR PARTNER THERAPY
The patient’s partner can be brought into individual treatment for a variety of reasons, both informational and therapeutic. Whether you invite him/her in occasionally or on a regular basis will depend on the value of the sessions.
On the informational side, having the partner involved in the treatment provides a different perspective on a variety of crucial issues, including providing information about
- the patient’s drinking, some of which your patient may not tell you.
- the patient’s other psychological and family issues.
On the therapeutic side, having the partner in offers an opportunity to
- deal with couple stresses.
- engage the partner in the therapeutic process.
- refer the partner out for individual work.
See Section 36 for a discussion of partner therapy. See Section 14 for a discussion of the pros and cons of partner therapy.
THERAPY FOR DEPENDENTS
There are many reasons to send dependents for their own treatment, including:
- Dependents are impacted by patient’s drinking, and need help coping.
- Dependents may not voluntarily come forward; but if they are sent for treatment, it may be helpful to them.
- The patient can be a role or behavior model for dependents, and they may need help separating or finding their own directions and goals.
Treatment of partners and dependents is discussed in Section 36.
FAMILY THERAPY
This is a flexible tool that can be used in a variety of ways, depending on the therapist’s training and interests. It requires a therapist with special training in family dynamics as well as pairwise relationships among individuals. For a discussion of the pros and cons of family therapy, see Section 14.
It may be helpful to have a few family sessions at times during individual treatment
- at the beginning of individual treatment with a patient, around issues of what family members fear, expect, and are willing to do to help.
- around disruptions in prior family behavior patterns and expectations.
- at times when the patient has a lapse and is at risk for relapse, to work out appropriate and effective reactions from other family members.
The concepts of family therapy often differ from those of individual therapy, and if you are considering an adjunctive referral for this form of treatment, it would be wise to confer with the proposed therapist in advance about the kinds of information you need and the kinds of interventions to expect. It is also important to maintain regular contact with the family therapist, both to share information and to coordinate treatment approaches. Some general comments about different approaches to family therapy can be found in Section 22.
GROUP THERAPY
Commonly this is the preferred primary method of treatment early on in recovery, as a way of helping the patient connect with others and feel less alone, while maintaining pressure to stay sober. It may become adjunctive as the patient changes and is able to make use of individual or family therapy as primary. For more about the pros and cons of group therapy, see Section 14.
If the patient’s issues are interpersonal, then a therapy group can provide an opportunity to confront them directly in a relatively safe environment. See Section 18 for more on group therapy.
Group therapy is generally less expensive than individual therapy, but it may not be covered by the patient’s insurance outside of a hospital or clinic setting.
19e Living and Working Conditions
Some patients may decide that their prior living conditions are too full of temptations to drink, and that they need to move to a safe residence for a period of time. A sober house is a place where recovering alcoholics and drug addicts can stay while they adjust to living without drugs or alcohol.
A sober house typically does not have the kinds of services that are found in rehabilitation centers. However, it does have rules for living, designed to support the person’s sobriety, facilitate living with others, reduce stress, and facilitate a return to normal living. Typical rules might include
- a curfew.
- no drugs or alcohol on the premises.
- no using drugs or alcohol at any time, on the premises or not.
- chores.
- having a job and paying rent.
- no sexual relations on the premises.
- all absences from the premises must be approved by the administrator.
- ongoing participation in an outside 12-step group.
If a person thinks he/she can benefit from such a setting, the first step is to call to see whether there is room. If so, he/she can ask for an interview to determine appropriateness. Typically, potential residents are screened for criminal history and must have a sponsor and the ability to pay rent. Expected time in the house is six months to a year, contingent on the person’s wish to stay and ability to meet the conditions of residence.
19f. Self-Help Groups
These provide information and support to people who are fighting to keep from drinking. In the early stages of recovery, there is no better way to break through denial than by the group process. There is no more credible group to an alcoholic than other alcoholics.
AA membership [ Section 16 ] is shown here as an adjunctive to psychotherapy for alcohol misuse. However, participation in AA or another self-help group is crucial to the treatment of most patients. Going to meetings can help a patient admit his/her problem, work on controlling the urge to drink, and move in more productive directions. It can also provide new awarenesses and stimulate new issues that can be dealt with in psychotherapy.
Once a person has attained sobriety, continued involvement in Alcoholics Anonymous [or another self-help group with a similar function] is crucial. It is a good idea to be aware of the person’s involvement, to ask about it regularly. Meetings can stimulate treatment issues, and advice from a sponsor can lead to patient reactions that are important to explore.
Early on in treatment, you may want to introduce an AA attendance sheet, that the patient must keep up to date, showing meetings attended, what s/he got from each meeting, etc. Use of such a sheet can enhance the patient’s commitment and involvement both with AA and with psychotherapy. If you detect a low level of commitment, you know to look at his/her resistance, and deal with it in some way. For example, if the person is socially phobic, you may arrange for someone to take him/her, or reassure him/her that it is OK to sit in the back at a meeting and just be there.
Many local self-help groups have national organizations that can be researched for their general principles of operation, assumptions, goals, etc. Section 16 provides brief discussions of a few of the better-known groups, including
- Alcoholics Anonymous [AA]
- Al-a-Teen
- Al-Anon
Among the many groups that are available, some might be more appropriate for a patient who sees his or her primary issue to be other than alcohol misuse. Al-Anon is directed to people who must deal with one or more alcoholics; ACOA is for children of alcoholics; and there are groups like Narcotics Anonymous for people whose primary addiction is to a chemical other than alcohol.
Alternative organizations include
- Life Ring
- Moderation Management
- Rational Recovery
- SMART Recovery
- Women for Sobriety
These groups are discussed in Section 16, which also includes a discussion of making the referral.
19g. Self-Help for Other Family Members
There are many reasons to suggest self-help groups for other members of the patient’s family: They need support in living with an alcoholic, and people in similar situations are happy to share their informed experience. Other family members may also have alcohol or drug problems, and support groups may help them deal with their own addictions.
The groups most commonly available and helpful are Al-Anon for adults and Alateen for adolescents. These and others are discussed in Section 16.
19h. Additional Treatment and Support
A major problem for recovering alcoholics is time management. Having a plan for getting through the day can help distract a patient from the urge to drink, give a reason to remain sober, and put him/her in regular contact with people and activities that support sobriety.
Many possible activities can be helpful here, including
- religious activities, meetings and events.
- hobbies.
- sports.
- political or social activities.
- volunteer work, e.g.: at a hospital, center on aging, parent-teacher group, etc.
In addition, other services are available which may be of special value to a person with a drinking problem. These include
- social services from the local county or state
- private or public legal help
- vocational or educational counseling
RELIGIOUS AFFILIATION
For some alcoholics, this can provide comfort, involvement with caring people, goals and direction, some services, and in some cases an opportunity to do paid or volunteer work. The latter may or may not be religious in nature.
Others may be unable to make use of what such groups have to offer for a variety of reasons: difficulties with organized religions, unavailability of groups of their own faith, being so self-critical that they feel out of place among religious people, etc.
HOBBIES AND ACTIVITIES
Developing an interest in a hobby or activity can help some people stay involved in non-drinking activities. Also, many hobbies or activities can include a social component that moves the patient away from situations involving drinking. Local newspapers may have listing of interesting groups and activities. The choice may be aided by the person’s history of past hobbies and activities.
SPECIAL TRAINING FOR DEFICITS
For many people, alcohol use may either serve as a crutch, to help them function socially, or it may isolate them and prevent them from developing or exercising social skills.
If they are successfully to abandon their reliance on drinking, they may need to learn new ways of coping in a social environment.
- Social Skills Training
- Stress Management
- Assertiveness Training
For more on these, see Section 25b.
SOCIAL SERVICES
The misuse of alcohol may have seriously disrupted a person’s life, to the point that he/she can’t function normally. He/she may have no place to live, no work, no friends or family, no form of transportation, etc.
A good place to refer the patient to for serious needs is the county department of social services. Here s/he can get money for medicine, food, and shelter, help in obtaining disability compensation, etc. Veterans can find help through local Veterans Administration centers.
LEGAL HELP
In Section 2, we considered the possibility that a patient might have been referred by the court system for alcohol-related legal difficulties. Whether or not this was the case, a patient’s misuse of alcohol could have led to legal complications: drunk driving, domestic violence, workplace complications, etc.
The person may need encouragement to obtain proper legal representation, and you may need signed releases to speak with the attorney.
If you plan to make the referral, it is a good idea to have a couple of attorneys in mind, who are sensitive to treatment issues and who can deal effectively with substance-related crimes.
VOCATIONAL OR EDUCATIONAL COUNSELING
A person who has misused alcohol for an extended period of time may have missed educational or vocational opportunities. The patient may have lost his/her job and have been unable to get another. His/her ability to set realistic career goals may have been impaired. A referral to an educational-vocational counselor can be very helpful to the person, in pulling his/her life together and moving in more positive directions.
Both public agencies and private counselors are available. They provide interest and vocational testing, information about careers and educational opportunities, and referrals onward to appropriate work or schooling.
OTHER CONTACTS THAT CAN BE HELPFUL
With the patient’s permission, you can also be in touch with
- agencies the patient is dealing with
- the patient’s physician
- the patient’s employer, religious leader, etc.
Explore for stress or support:
- —Living conditions
- —Neighborhood
- —Work setting and pressures
19i. Choosing Adjunctive Care
There are many possible goals of adjunctive care, depending on the needs of the patient and his/her family. Adjunctive care can furnish treatment and additional services that can’t be provided by the primary form of treatment. Your choice depends on the needs of the patient and the limits of the primary method of treatment. Any choice may be tentative and change with time as the patient changes.
AND PRIMARY FORM OF TREATMENT
An adjunctive treatment should be different enough from the primary treatment modality to minimize duplication of effort and splitting of the transference.
If the primary form of treatment is individual psychotherapy, you would generally not want to send a patient for regular consultations with another professional who is quick to provide psychological advice. If the primary form is group therapy, you might be hesitant to send the person to a self-help group and might instead refer out to individual psychotherapy or a self-help sponsor. On the other hand, the group therapy might be distinctive enough from self-help groups that the two forms supplement each other.
AND PATIENT FEARS OR LIMITATIONS
Here the issues have to be explored as they come up, generally by making a suggestion and noting the person’s reaction to it.
Some people are afraid of groups – because they are shy and fear exposure, or self-critical and fear being found out, or fear that the group will pressure them to do things they might not want to, etc. For these, group therapy or self-help groups may seem too risky to try. A judgmental patient may fear being judged by others in a self-help group or become so judgmental of them that the value of the group is lost.
Some people avoid physicians and psychiatrists because of an aversion to taking medications. They sometimes seem shocked at the idea that alcohol is itself a form of medication that they have been self-prescribing – ineffectively – themselves.
With any fear, you can explore the nature of the fear, provide new information, and possibly persuade the person to try the feared treatment.
AND STAGE OF CHANGE [see Section 40 ]
A person who is in the precontemplation stage probably isn’t ready for any of this relative to alcohol treatment, unless he/she is compliant or submissive and will go for the treatment because he/she has been told to do so.. If the person is in another stage relative to another issue, the choice of adjunctive care may depend on treatment of that issue.
A person in contemplation or preparation will need adjunctive care that supports change. A person in the action stage can make use of more direct adjunctive care related to alcohol treatment
AND STAGE OF RECOVERY
Early in recovery, the goal of getting the person on his/her feet and supporting abstinence are primary. Self-help groups, religious s affiliations, social services, group therapy, and possibly legal help are all important.
Later on, as the person stabilizes and needs to redirect his/her life toward more productive goals, vocational counseling, hobbies and activities become increasingly helpful.