-
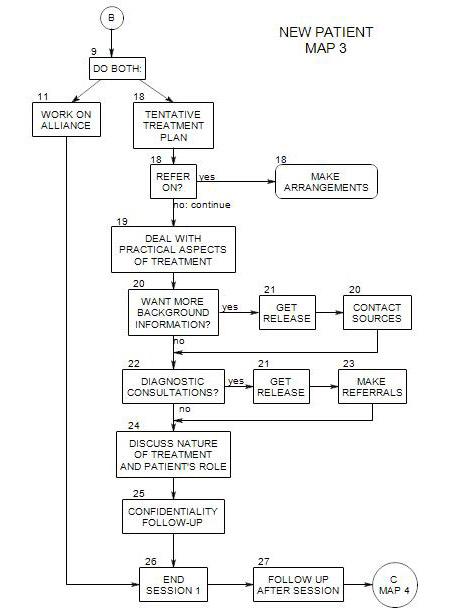
Appears on Map 3 after Section 26
Refer to Section 3 for more on HIPAA
27a. Review Session
It’s a good idea to go over the session soon after the patient leaves, to organize your thoughts and records. You can write notes on the session or, if you were taking notes during the session, re-organize them. You can make a list of additional information you would like to have, confusing things said, etc.
27b. Enter the Patient into your Billing System
After the first session, you should already know-
- whether there is insurance and/or managed care.
- how to contact important financial third parties
- enough information to bill the patient and hihe/sher insurance company, if needed
- how often to expect this person
This information should be organized for easy access and filed away
27c. Begin Organizing Your Information about this Person
Separate your session notes from billing data and other personal health information about the person. Keep the two sets of information in different places [eg: different folders, in different parts of your file cabinet].
Begin a summary record of treatment, that contains important information you will want to refer back to.
Begin working on a preliminary diagnosis – either an very informal one that can guide your next treatment steps, or a formal one that can inform third parties that the person is in need of professional help, or both.
Make sure that all this information is secured, either in locked cabinets or pass-protected computer files.
27d. Verify Insurance Coverage and Initiate Treatment with Managed Care
This needs to be done quickly, to determine
- whether the patient has insurance coverage, and if so, the terms of coverage. If not, alternative payment arrangements must be made, and it probably is in your best interest to make them before the next session.
- whether the patient’s insurance will pay for treatment with you. If not, then you must either join the panel, arrange alternative payment, or refer the person on to another therapist
Any delay in dealing with these issues could lead to unnecessary tension in the treatment and/or loss of income for you.
For indemnity [not-managed] insurance, important information to gather includes:
- Whether the person is currently covered by the policy he/she thinks is covering
- The annual deductible [which presumably the patient will pay]
- The amount paid per session. [subtract this from your fee to get the patient’s payment]
-
Total coverage per year or per episode
- What, if anything other than psychotherapy [eg: psychiatric consultation] is included in the annual total
For patients whose insurance is managed, you might also want to know
- Whether you are a member of the treatment panel; and if not, then whether you can either become a member quickly or see the patient on a single case basis. In the latter circumstance, you may have to justify treatment with you on grounds that in-network providers are unavailable or lack your experience with the patient or treatment skills.
- Whether initial case registration is needed prior to treatment.
- When you must provide the first Outpatient Treatment Report, and how to get the necessary forms.
- Where to send OTR’s.
27e. Contact the patient’s physician
If you decide to do this, you will typically make a call to the physician’s office, Indicate that you need information about your shared patient, and arrange to send a copy of the release you have already obtained.
Ask about the patient’s medical history, especially about medical conditions that might lead to the symptoms you have observed or the patient has complained of. Lists of likely conditions are provided in the specialty maps.
Also ask about any medications that may be currently prescribed for the patient, including doses and the physician’s awareness of compliance issues, if any. Partial lists of medications that can cause or exacerbate psychological disorders can be found in the specialty maps.
One way to cover a lot of possibilities would be to ask the physician personally for any conditions that could be symptom-related, then send along a checklist with your written request for records, that his/her assistant could fill out and return.
27f. Contact consultants
This is only called for if you decide to refer the person to a specialist for relevant information that the person can’t provide, the person’s physician doesn’t have, and you can’t gather yourself.
This could happen if the person needs specialized psychological tests, vocational counseling, alcohol treatment, etc. You might also want to refer for tests for medical conditions and/or an opinion about the effectiveness of certain medications in alleviating the person’s symptoms.
When you refer on for consultations, you will want to have a list of questions for each consultant, based on his/her relationship to the patient and the kind of information he/she is likely to be able to provide. Sometimes your new perspective can be helpful to the other specialist also, in suggesting new approaches or explanations.